Male Reproductive System
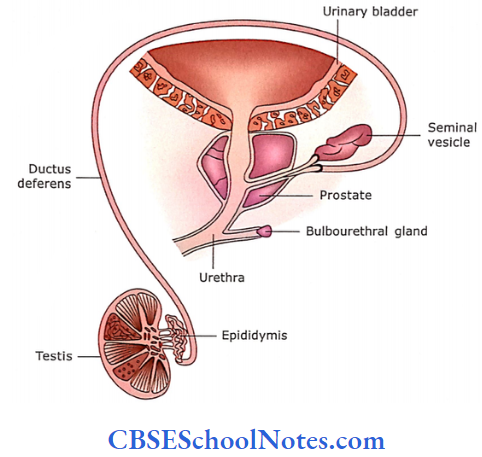
The testis is the main organ of reproduction in males. It is involved in the production of sperm and testosterone. The accessory organs are the epididymis, ductus deferens (which convey the sperm from the testis to the prostatic part of the urethra) and penis (a copulatory organ).
During the passage of sperm from the testis to the penis, accessory glands like the seminal vesicle, prostate and bulbourethral glands provide a fluid vehicle for sperm and make them more motile.
Testis
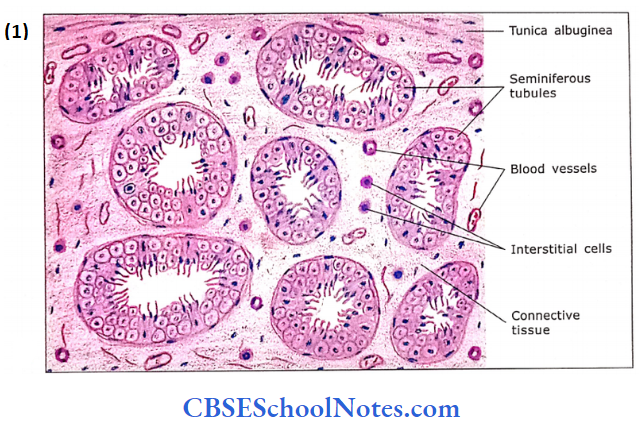
The testes lie outside the body cavity in the scrotum. They are ovoid and measure approximately about 5 cm in length and 2.5 cm in diameter. Each testis weighs 10-15 g. The testis has a thick white fibrous connective tissue capsule called the tunica albuginea.
The tunica vasculosa is a highly vascularized connective tissue, which underlies the tunica albuginea.
- On the posterior border of the testis, the dense connective tissue of tunica albuginea projects into its interior and forms the mediastinum of the testis.
- Through the mediastinum, blood vessels, nerves and ducts of the testis enter and leave the organ.
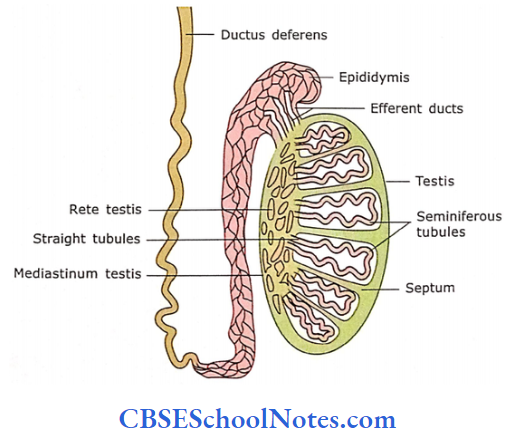
- The connective tissue septa extend between mediastinum and tunica albuginea and divide the testis into about 250 compartments called as lobules
- Each lobule contains one to three tightly coiled tubules, the seminiferous tubules.
- Thus, each testis contains more than 500 seminiferous tubules. Each seminiferous tubule is about 30-70 cm long and about 200 cm in diameter.
- These tubules are sites where sperm are produced. Sperms are produced in these tubules.
- In between seminii- erous tubules, there is the presence of loose connective tissue (interstitial tissue) and blood vessels.
- The interstitial tissue contains endocrine cells, Leydig cells or interstitial cells, which produce testosterone.
- At the apex of the lobule, near the mediastinum, seminiferous tubules open into tubuli recti, which connect the open end of each seminiferous tubule to the rete testis.
Rete testis are epithelial-lined labyrinthine spaces within the mediastinum testis. The spermatozoa after passing through rete tesis travel through 10-20 short tubules known as efferent ducts. These efferent ducts fuse with epididymis.
Testis Remember:
The main function of testes is to produce spermatozoa and synthesize the hormone testosterone.
Microscopic Structure Of Testis
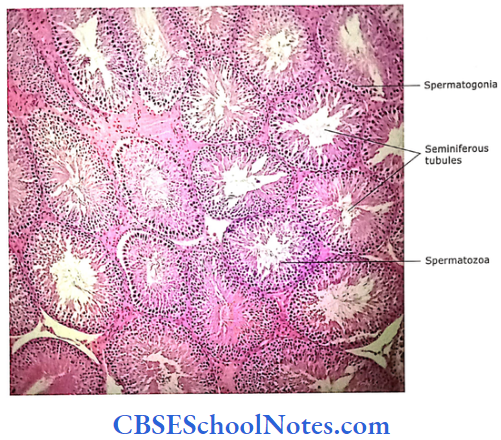
The testis consists of seminiferous tubules, interstitial tissue and blood vessels.
Seminiferous Tubules
Each seminiferous tubule is long and convoluted. It is surrounded by a layer of connective tissue called lamina pro-pria. This layer consists of flattened or spindle-shaped myoid cells arranged in one or more layers. The myoid cells are contractile and help spermatozoon and testicular fluid to move through seminiferous tubules. Deep into lamina propria is basal lamina.
A dense capiUan network surrounds each seminiferous tubule- A dense capillary network surrounds each seminiferous tubule. Deep into lamina propria is basal lamina. On the basal lamina, seminiferous tubules are lined by a complex stratified epithelium.
Which contains two major cell classes.
- Supporting cells and
- Spermatogenic cells.
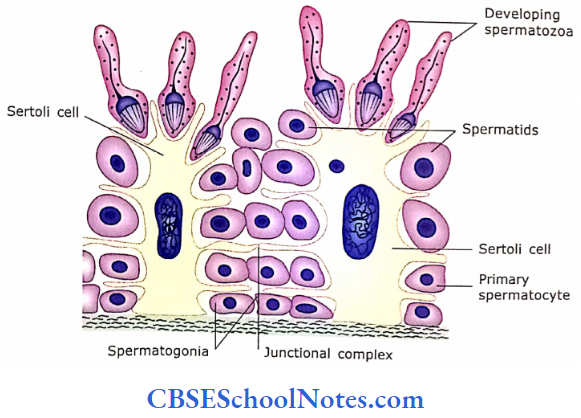
1. Supporting Cells (Sertoli Cells)
Sertoli cells are tall columnar cells, which extend from the basal lamina to the free surface of the epithelium (lumen of tubule). These cells have irregular outlines as they have lateral cell processes, which surround all spermatogenic cells except those resting on basal lamina. Sertoli cells are non-dividing cells in adults. They have ovoid euchromatic nuclei with one or more prominent nucleoli.
Sertoli cells Ultrastructure:
The Sertoli cells exhibit faint longitudinal striations.
- The cell has a meshwork of thin actin filaments, bundles of intermediate filaments and microtubules arranged parallel to the cell axis.
- These filaments and microtubules are involved in the change of shape of Sertoli cells that help in the movements of the germ cells toward the surface.
Sertoli cells Functions:
Sertoli cells provide mechanical support to the spermatogenic cells.
- They provide nutrition to the spermatogenic cells.
- Sertoli cells form a blood-testis barrier, thus preventing the movement of extracellular molecules into the seminiferous epithelium.
- They also secrete some components of testicular fluid.
Blood-Testis Barrier:
Complex intercellular tight junctions are present between lateral processes of Sertoli cells over spermatogonia. The inter-sertoli junctions comprise a “blood-testis barrier” to prevent sperm-related proteins from entering the circulation.
The blood testis barrier serves an important role in isolating developing sperm cells and spermatozoa from the immune system. This prevents the formation of sperm-specific antibodies.
- These junctional complexes divide the seminiferous epithelium into two compartments, i.e., basal and luminal.
- The basal compartment is present between basement mem¬brane and junctional complexes. It contains spermatogonia and primary spermatocytes.
- In the luminal compartment, secondary spermatocytes and spermatids are present.
- The movement of primary spermatocytes from the basal com¬partment to the luminal compartment takes place by the formation of new junctional complexes beneath the primary spermatocytes.
- Once the secondary spermatocyte is formed then the junctional complex situated above the dividing pri¬mary spermatocytes break down and spermatocytes move to the luminal compartment.
- Thus, the junctional complexes separate the antigenic haploid germ cells (secondary spermatocytes, spermatids and sperms), which are present in the luminal compartment form the immune system of adults. This prevents the formation of sperm-specific antibodies.
Sertoli cells Remember:
The Sertoli cells serve many functions, i.e., form the blood testis barrier; secrete androgen-binding proteins and hormones; provide support and protection to spermatoge¬nic cells, and provide nourishment to developing sperm. Sertoli cells also phagocytose cytoplasmic remnants of spermatids
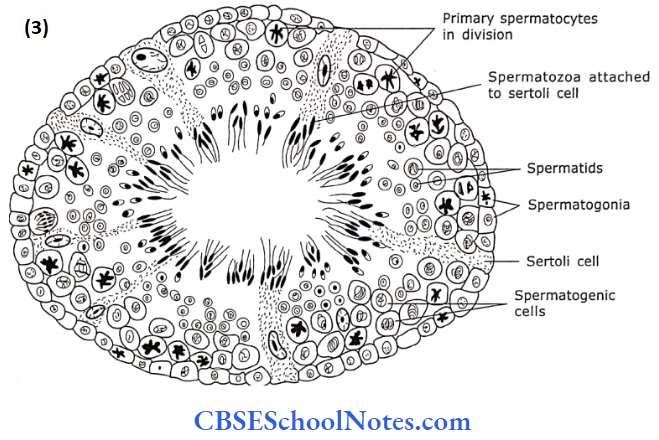
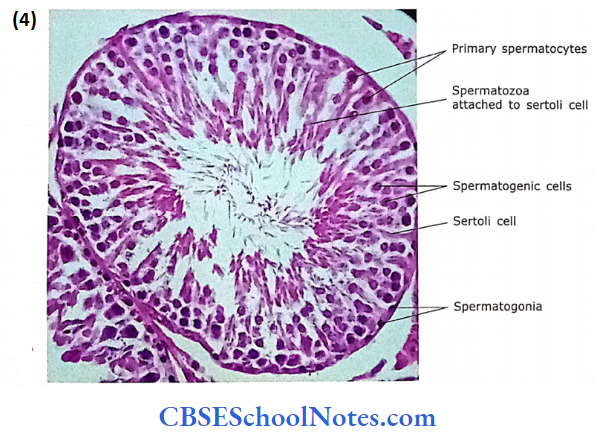
2. Spermatogenic Cells
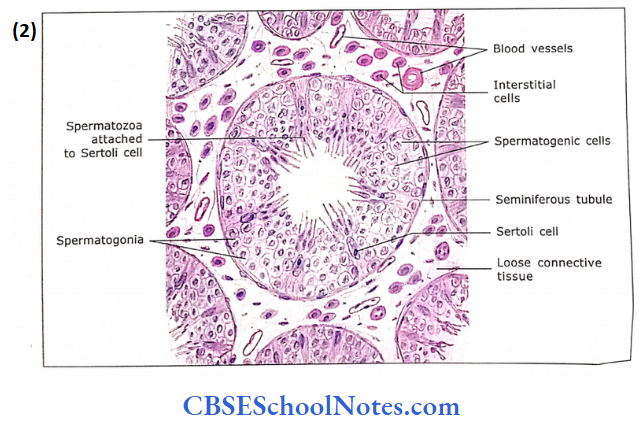
Besides Sertoli cells, the seminiferous tubules are also lined with spermatogenic cells. The spermatogenic cells are arranged as complex stratified epithelium and consist of stem cells (spermatogonia) at the base of the epithelium.
- The other cells at successively higher levels are primary spermatocytes, secondary spermatocytes, spermatids and spermatozoa. These cells are in different stages of differentiation of sperm.
- Thus seminiferous tubule consists of two different cell populations, i.e., Sertoli cells and a population of germ cells.
- The germ cells (spermatogonia) divide at the base of the epithelium and slowly move upward while they differentiate into spermatozoa.
- The spermatozoa are then released into the lumen of the seminiferous tubule.
- The spermatogenesis is under the control of pituitary hormones, luteinizing hormone (LH, ICSH) and follicle-stimulating hormone (FSH).
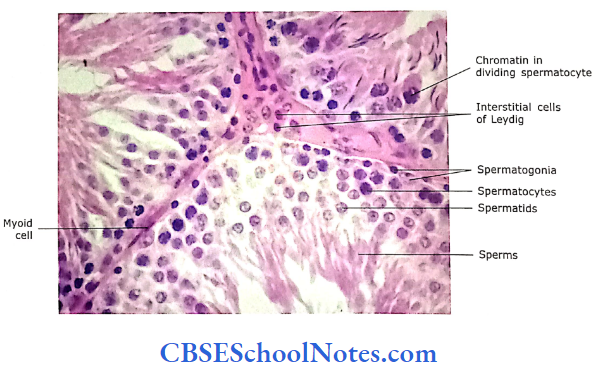
Interstitial Tissue and Blood Vessels:
In between the seminiferous tubules are many fenestrated capillaries, lymphatics, loose connective tissue and Leydig (interstitial) cells. The blood vessels apart from the usual function of blood supply, supply cooler blood to the testes.
- The heat of the testicular artery is partly dissipated by its proximity to the pampiniform plexus of veins, which carries cooler venous blood from the testis and surrounds the artery in the spermatic cord.
- The extra-abdominal scrotal position and dartos muscle also regulate the temperature of the testis.
- Leydig cells are 3-8 pm in diameter. They are acidophilic, polyhedral in shape and found in clusters. They secrete testosterone.
- Testosterone stimulates spermatogenesis by influencing the Sertoli cells. It also supports the structure and functions of the accessory sex organs and ducts.
- Testosterone is also responsible for male secondary sex characteristics.
Seminiferous tubules Remember:
Seminiferous tubules consist of complex stratified epithelium surrounded by a thin connective tissue layer, i.e., lamina propria. The epithelium is composed of two different types of cells, i.e., Sertoli cells and spermatogenic cells.
Mature Spermatozoon:
The mature spermatozoon is commonly considered to have a head, neck and tail
- Head: The nucleus having condensed chromatin is covered in front by the acrosome. The acrosome is later released at the time of fertilization to disperse the corona radiata and digest the zona pellucida of the ovum.
- Neck: It is a short segment containing the centriole that gives rise to the core of the flagellum (9+2). or axoneme.
- Tail: The tail has 3 pieces, i.e., midpiece, principal piece and end piece. The mid piece is 5-7 urn in length. Here. 9 coarse fibres form a sheath around the flagellar core. Mitochondria become helically condensed around the sheath, which provides energy for sperm motility. The principal piece is about 45 pm in length. The axoneme and 9 coarse fibres are enclosed in a fibrous sheath. The end piece, 5-7 urn long, consists of axoneme enclosed by plasmalemma.
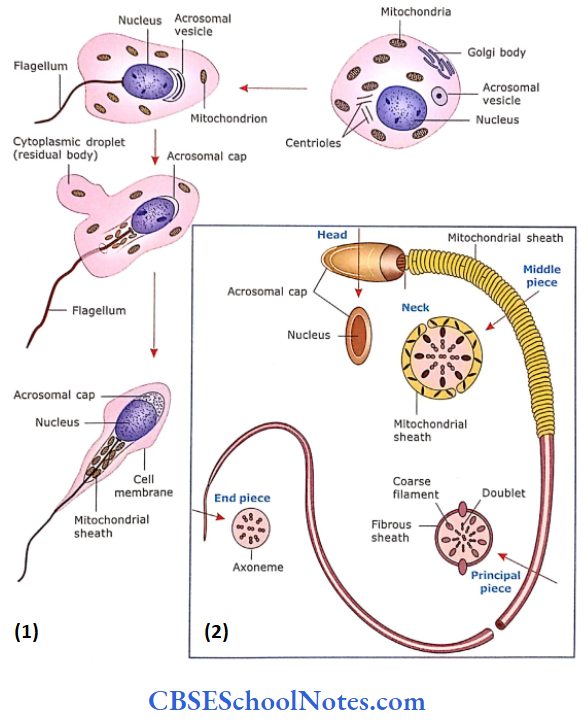
Spermatozoon Remember:
The spermatozoon consists of the head, neck and tail. The head consists of a nucleus while the tail is divided into three regions, i.e., midpiece, principal piece and end piece. The head is about 5 μm long, while the tail is approximately 55 μm in length.
Sperm Clinical Application
- Immotile Sperm: Sperms are highly motile in the female genital tract.
- However, in a condition known as immotile cilia syndrome, sperm are unable to move from one place to another.
- This results in infertility.
- The immobility of sperm is due to the absence of protein (dynein) required for the motility of cilia and flagella. This also affects the cilia present throughout the body.
- Thus, immotile cilia syndrome is also associated with chronic respiratory infections because of the presence of immotile cilia on the respiratory epithelium.
- Sperm-specific Antibodies: The secondary spermatocytes, spermatids and spermatozoa possess specific proteins, which are recognized as foreign by the body.
- Usually, these proteins are isolated by the blood testis barrier.
- However, in case of breakage of the immune barrier there occurs the formation of sperm-specific antibodies.
- These antibodies agglutinate the sperms, thus preventing their movements. This leads to infertility.
- This kind of infertility can be detected by estimating the level of anti-sperm antibodies in the blood serum.
Duct System
The duct system of the male reproductive organ consists of the following tubules or ducts.
1. Straight Tubule (Tubuli Recti)
- Straight tubules are the final portions of seminiferous tubules. The proximal part of the tubules is lined with simple columnar cells and Sertoli cells. The distal part is lined by simple cuboidal cells with microvilli.
2. Rete Testis
It consists of a system of flattened anastomosing channels in the dense connective tissue of the mediastinum that drains the straight tubules. The rete testis is lined by low cuboidal epithelium with microvilli and a single flagellum.
3. Efferent Ducts
- They collect the sperm from the testis. Efferent ducts consist of 12-15 coiled tubes that coalesce to form the head of the epididymis.
- The lumens of ducts are wavy in appearance.
- This is because these ducts are lined by alternating groups of simple ciliated columnar and groups of cuboidal cells. The cilia of columnar cells propel the still non-motile sperm.
- Cuboidal cells are probably absorptive.
- Beneath the base membrane, in lamina propria, a thin layer of circular muscle is present.
Duct system Remember:
Tubuli recti (straight tubule) and rete testis are present within the testis and both are lined by low cuboidal cells with microvilli. The efferent ducts are interposed between the rete testis and epididymis.
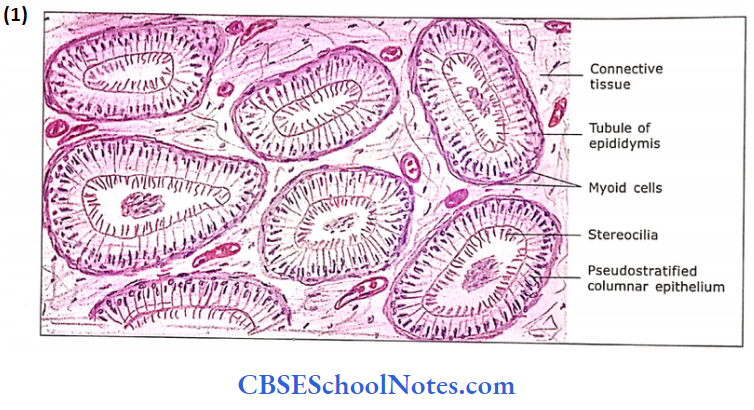
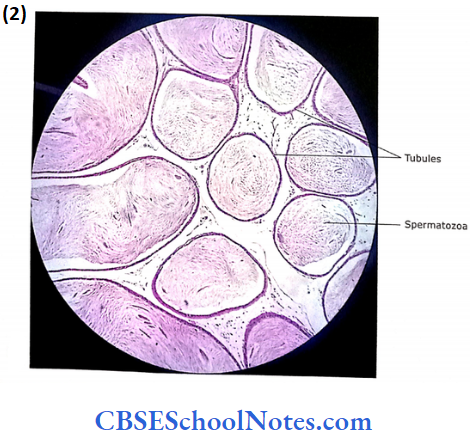
4. Epididymis
Efferent ducts fuse to form this 20-foot-long, highly coiled tube, which can be divided into head, body and tail.
- The epididymis is placed at the posterior border of the testis. The whole organ and individual tubes are surrounded by vascular connective tissue.
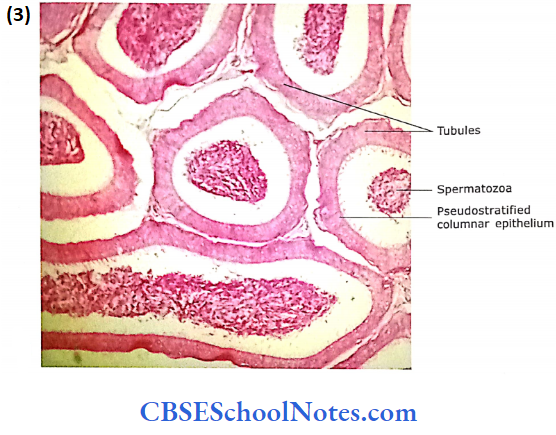
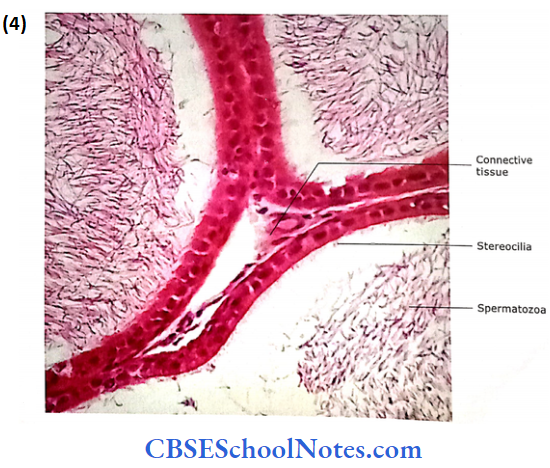
- The lining of the tubule is the pseudostratified epithelium. It consists of low basal cells and tall columnar cells. The tall columnar cells are with long stereocilia.
- The function of epithelium is not well understood as stereocilia are non-motile. Probably, the epithelium is involved, both in secretion and absorption.
- The lumen of the tubule may show the collected sperms. Beneath the distinct basement membrane, lamina propria contains circularly arranged smooth muscle fibres.
- The smooth muscle helps to push the sperm along, especially in the proximal segment.
Epididymis Functions
The epididymis is so long that it may take a month for sperm to make the journey.
- The distal or tail segment stores the sperms, where they mature and lose the last bit of cytoplasm attached to their head and middle piece and become motile, thereby acquiring the capacity to fertilize an ovum.
- Smooth muscle in the wall contracts rhythmically during ejaculation to move the sperm along.
- It also contributes a viscid nutritive substance.
- The epithelial cells of epididymis also phagocytose the degenerated sperms and residual bodies.
Epididymis Remember:
Epididymis is formed by the fusion of efferent ducts. It is a highly coiled tubule divided into head, body and tail. The tail of the epididymis is continuous with ductus deferens. Within the epididymis sperms are stored, mature and thereby acquire the capacity to fertilize an ovum.
5. Ductus Deferens
It is a thick muscular tube extending from the tail of the epididymis to the prostatic part of the urethra. It drains the epididymis.
The ductus deferens consists of the following layers in its wall:
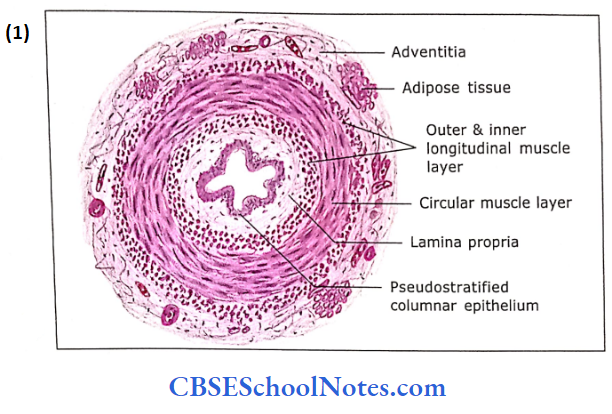
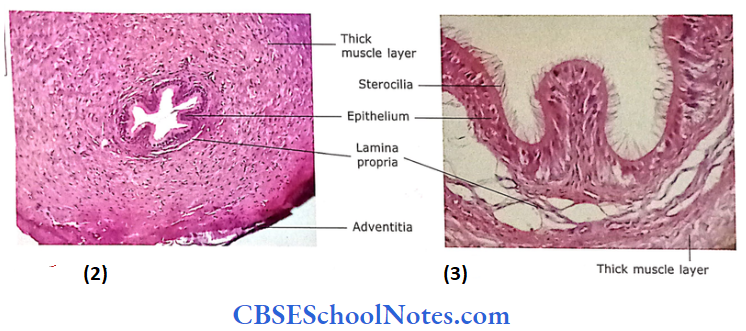
- Mucosa: The lumen of the duct is irregularly star-shaped. The epithe¬lium is pseudostratified columnar with stereocilia and resembles that of epididymis. The lamina propria underlying the epithelium contains collagenous and elastic fibres.
- Muscle Layer: It consists of three layers of smooth muscle, i.e., outer and inner thin layers of longitudinal muscle and a well-devel¬oped thick middle layer of circular muscle. The muscle layer is very thick (1-1.5 mm) compared to the thickness of the mucosa.
- Adventitia: The adventitia is made up of loose areolar tissue, which contains many blood vessels and nerves. The terminal part of the ductus deferens is dilated to form an ampulla. Here, the mucosa is thrown into tall branching folds covered by a low columnar epithelium.
Ductus deferens Functions
- The ductus deferens does not store sperm.
- The duct is involved in rapid propulsion during ejaculation because of its strong musculature.
Ductus deferens Remember
The wall of the vas deferens consists of three layers of smooth muscle. This strong musculature helps in the propulsion of sperms from the tail of the epididymis to the ejaculatory duct during ejaculation.
Accessory Sex Glands
1. Seminal Vesicle
The seminal vesicles are elongated sac-like structures with a highly convoluted irregular lumen. Each gland consists of. single tube, about 3-1 mm in diameter, 12-15 cm m light,
Which is folded upon itself to measure about 5 cm in length. It joins with the ductus deferens to form an ejaculatory duct The wall of the seminal vesicle is composed of the following three layers
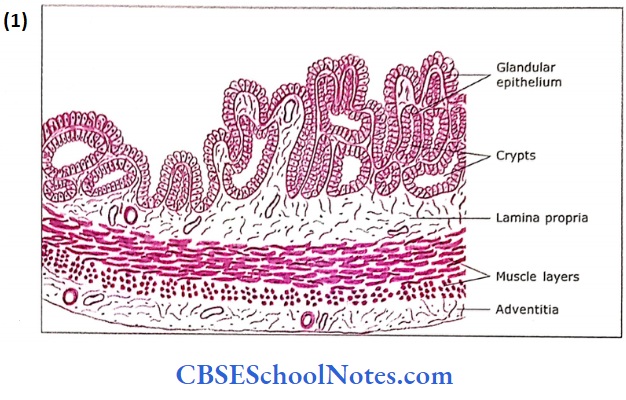
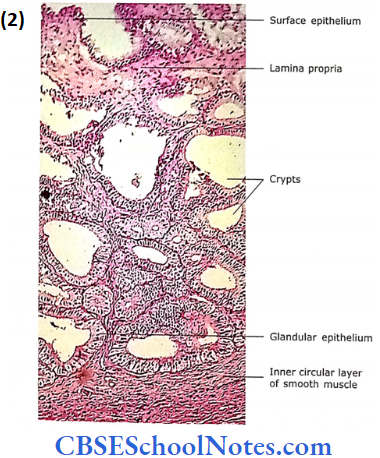
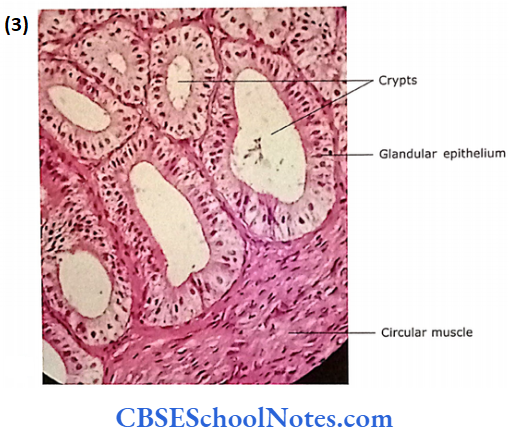
- Mucosa: The mucosa is thrown into highly complex folds.
- These folds join with each other to form many crypts and cavities.
- The core of these folds is formed by connective tissue derived from lamina propria. The lamina propria is rich is elastic fibres.
- The epithelium is pseudostratified low columnar or cuboidal. In some places, epithelium is simply columnar or cuboidal.
- These cells are secretory. The epithelium varies greatly in height and appearance with activity, blood testosterone level and age.
- Muscle Layer: The muscle layer is made up of smooth muscle, which is thinner than that of ductus deferens. The muscle is arranged in two layers, i.e., inner circular and outer longitudinal. The contraction of the muscle at the time of ejaculation expels the secretion of the gland into the ejaculatory duct.
- Adventitia: A thin layer of loose connective tissue surrounds the muscle layer.
Seminal Vesicle Functions
- The gland secretes seminal fluid, which is a yellow viscous fluid containing fructose (an energy source for sperms) and prostaglandin.
- The seminal fluid is alkaline in nature.
- The pale yellow colour of semen is due to lipochrome pigment released by seminal vesicles.
- The gland is under the control of androgen. It helps to flush the sperm out of the urethra.
Seminal Vesicle Remember:
The seminal vesicle is not involved in the storage of sperm. It secretes a yellow viscous fluid that contains fructose and prostaglandin and constitutes about 70% of ejaculate.
2. Prostate Gland
The prostate is the largest of the accessory glands. It is about the size of the chestnut. It surrounds the first part of the male urethra after it emerges from the bladder.
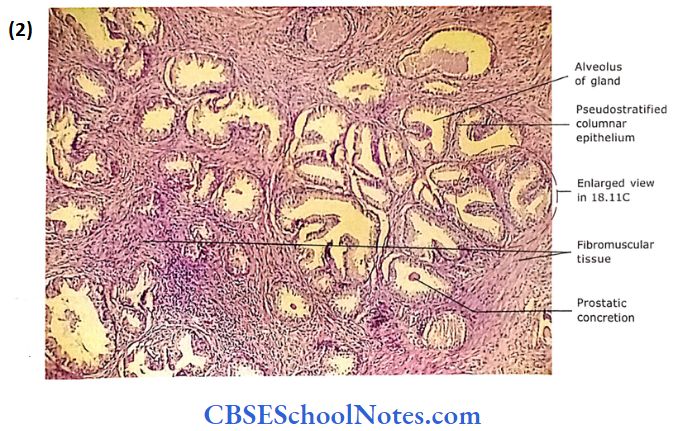
- It is comprised of 20-50 tubulo-alveolar glands, which open by 15-25 ducts into the prostatic urethra. The stroma of the gland consists of fibromuscular tissue in which glandular tissue is embedded.
- Thus, the prostate is known as a fibro¬muscular glandular organ. The prostate gland is surrounded by a thick capsule.
- Three groups of glands surround the prostatic urethra concentrically, i.e., mucosal, sub-mucosal and main prostatic gland. The mucosal glands are small tubular glands situated in the mucosa, which open directly into the prostatic urethra.
- The submucosal glands are situated deep in the mucosa and are tubulo-alveolar type.
- The prostatic glands are situated in the outer zone of the prostate. Both submucosal and main prostatic glands open through long ducts into the prostatic urethra.
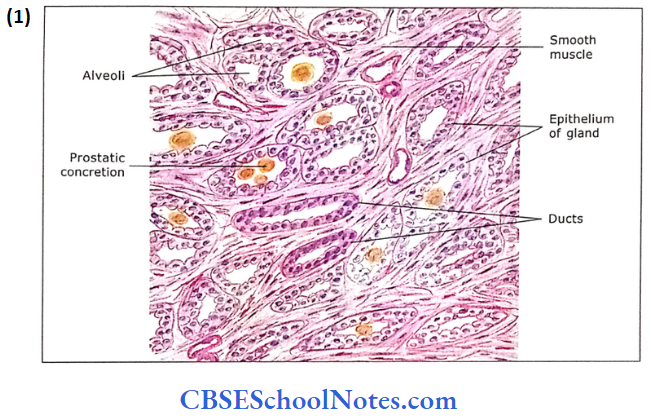
- The alveoli of the glands are surrounded by the fibromuscular stroma. The stroma consists of smooth muscle, collagenous and elastic fibres.
- The fibro-muscular stroma runs in different directions and contains blood vessels, lymph vessels and nerves. The glandular alveoli are of variable sizes and irregular lumens.
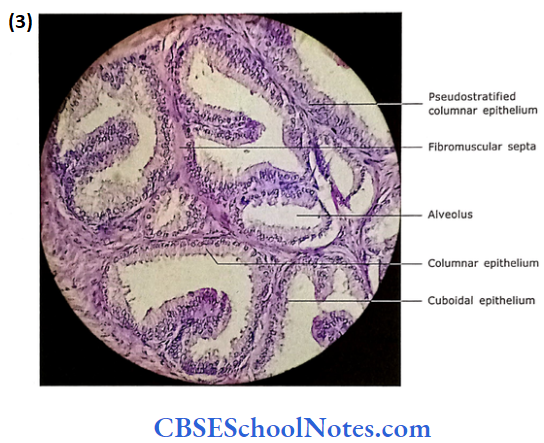
The epithelium lining the alveoli is secretory. It is either a simple columnar or a pseudostratified columnar.
- However, in some places, the epithelium may be low cuboidal. The variation in the epithelium (low cuboidal to pseudostratified co¬lumnar) is due to its functional state.
- In old people, the lumen of some of the gland alveoli may show the presence of prostatic concretions (corpora amylacea), which are oval-dense bodies of glycoproteins
- This results from to condensation of secretory products, which may become calcified. The significance of these bodies is not known.
- The prostatic urethra, above the opening of ejaculatory ducts, is lined by transitional epithelium. The lower part of the prostatic urethra is lined by stratified columnar epithelium
- . The epithelial lining is surrounded by lamina propria and outside by smooth muscle.
Prostate Gland Functions
- The prostate secretes 10-30% of final ejaculate.
- The fluid is thin and contains acid phosphatase, citric acid, amylase, fibrinolysin and prostate-specific antigen (PSA). Fibrinolysin helps in liquefication of semen.
- Prostatic secretion is facilitated by the contraction of smooth muscles of the stroma at the time of ejaculation.
- Prostatic secretion promotes the mobility of sperm.
Prostate Gland Remember:
Three groups of glands surround the prostatic urethra concentrically, i.e., mucosal, sub-mucosal and main prostatic gland. The prostatic secretion contains acid phosphatase, citric acid, amylase, fibrinolysin and prostate-specific antigen (PSA). Fibrinolysin helps in liquefication of semen.
Prostate Gland Clinical Application
- Enlargement of Prostate:
- The glandular tissue of the prostate starts proliferating after 40-45 years of age in almost 50% of men. However, 80% of males are affected by 70 years of age.
- The enlarged prostatic tissue compresses the prostatic urethra, which leads to difficulty in passing urine.
- The disease is called benign prostatic hypertrophy. It can be treated by surgical removal of a part of the gland.
- The malignant prostatic tumour is the second most common cancer in men. The tumour arises from glandular tissue of the prostate gland, hence called as adenocarcinoma of the prostate.
- The level of PSA increases in cancer of the prostate and is used for early detection of cancer. In this case, complete removal of prostate is required.
Bulbourethral Gland
The bulbourethral glands (Cowper’s gland) lie in the urogenital diaphragm and empty into the proximal portion of the penile urethra The gland is about the size of a pea. It discharges a mucus-like lubricant. It is a compound tubuloalveolar gland. The epithelium of the secretory part varies from simple cuboidal to simple columnar.
3. Bulbourethral Gland Clinical Application
- Semen: The semen contains spermatozoa and secretion of acces¬sory sex glands. The volume of the ejaculate is about 3 mL, 95% of which is secretions from accessory glands. The sperm concentration varies from 50 to 250 million/mL. A male whose sperm count is less than 20 million/mL of ejaculate is considered as sterile.
- The following glands contribute to the formation of semen:
- Bulbourethral Gland: The secretion is mucus-like fluid, which acts as a lubricant. Secretion starts appearing much before ejaculation begins.
- Prostate Gland: The secretion of the prostate coagulates the semen, which is later liquefied by fibrinolysin.
- Seminal Vesicle: The secretion is rich in fructose, which provides energy to sperms.
- Impotence:
- The inability to achieve an erection is called as impotence.
- I Impotence may be temporary or permanent. The temporary impotence may be due to drugs or psychological factors.
- The permanent impotence is due to lesions in the brain, hypothalamus, and spinal cord and injury to autonomic nerves.
- It may be also due to various systemic diseases such as multiple sclerosis, Parkinson’s disease and diabetes
Bulbourethral Gland Remember:
Secretion of the bulbourethral gland acts as a lubricant and its release in the urethra is due to sexual stimulation.
Penis
The penis is an erectile copulatory organ. It is a common organ through which both semen and urine are discharged. The penis is made up of three cylindrical bodies of erectile tissue
The corpora cavernosa are placed dorsally while a single corpus spongiosum is placed ventrally.
- The urethra passes within the corpus spongiosum and opens at the tip of dilated part of the penis called as glans penis. The glans is covered with a fold of skin called a prepuce.
- In the shaft of the penis, each of the three erectile bodies is covered by a thick connective tissue sheath called the tunica albuginea.
- The tunica albuginea also fonus an incomplete partition between two corpora cavernosa. The tunica albuginea is covered with a layer of loose connective tissue and skin.
- A cross-section of the penis shows the following structures from superficial to deep. The most superficial structure is thin skin, which is devoid of any hair.
- Deep to the skin is the presence of a loose connective tissue layer, which is devoid of fat (adipose tissue). This layer of loose connective tissue is also called Buck’s fascia.
- It binds the tunica albuginea of all three erectile tissues with each other. Deep to this, the tunica albuginea covers all three erectile cylindrical bodies, i.e., two dorsal corpora cavernosa and one ventral corpus spongiosum.
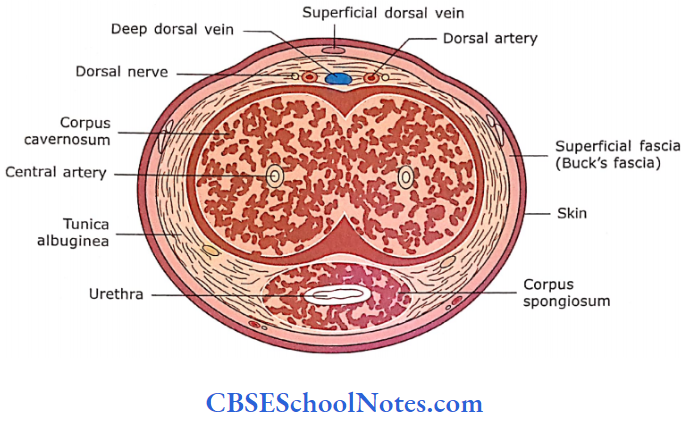
The erectile tissue of the corpora is a sponge-like mass of endothelial-lined vascular spaces. The walls of these spaces are formed by numerous.
- Trabeculae consist of collagen fibres, elastic fibres and smooth muscle. These spaces are supplied by afferent arteries, which are branches of central deep arteries. T
- these spaces are drained to veins on the inner aspect of the tunica albuginea. They penetrate the tunica obliquely to join the deep dorsal vein of the penis.
- During the erection of the penis, blood fills the cavernous vascular spaces because of the vasodilation of arteries due to psychic and afferent sensory input.
- These spaces expand as they are filled with blood under pressure.
The peripheral veins are compressed against the inner surface of tunica albuginea, hence blood outflow diminishes considerably. This causes the erection of the penis. Erection is controlled by the parasympathetic nervous system, while ejaculation is controlled by the sympathetic nervous system
The corpus spongiosum is traversed by the penile urethra throughout its length. The urethra is lined by stratified columnar or pseudostate-tied columnar epithelium. The tip of the urethra, at the glans penis, is lined by stratified squamous non-keratinized epithelium. There are many small mucous glands of Eittre, which are scattered along the length of the urethra. They secrete mucus and have e lubricating function.
Penis Remember:
Filling of cavernous spaces (corpora cavernosa and cor¬pora spongiosum) with blood causes the erection of the penis.
